It has been a hard couple of weeks for Obamacare. The law’s online marketplaces — where people were supposed to be able to easily shop for health insurance — have been suffering from high-profile defections and double-digit premium increases.
Critics of Obamacare have pointed to the recent problems as proof the market is not working, while even the law’s staunchest defenders are arguing that the marketplaces need some fixes. Here are four key challenges to the program and a survey of some possible solutions.
Choice is disappearing
The problem: The insurance co-ops created by the law have mostly gone belly-up. UnitedHealth bowed out of most states where it offered individual plans on the exchanges. Aetna pulled out from 11 states. And smaller carriers, like the start-up Oscar Health, which has been struggling, have reduced their footprint.
Three years in, many established insurers say they are seeing their losses from selling individual plans deepen. Many of the nonprofit Blue Cross plans and other well-regarded insurers, like Geisinger Health, are having trouble. There is something of a herd mentality taking place — if all my competitors are leaving, maybe I should, too.
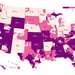
Continue reading the main storyWhy it’s a problem: Competition, at least in theory, helps keep premiums low and service high. That’s the whole point of having a market for health insurance. But 17 percent of people eligible for this market might have no choice of carrier next year.
Possible solutions: If the market looks as if it’s growing and stable, some insurers might come back. Both President Obama and Hillary Clinton have also revived the idea of the so-called public option, which would be a government-run plan that would either compete with or be a substitute for a plan offered by a private insurer. It’s politically controversial and hard to make work in practice.
Prices are rising
The problem: Everyone is anticipating a much bigger price increase for Obamacare plans next year than in the past.
Why it’s a problem: People who do not receive federal tax credits to help pay for their coverage are particularly hard hit by having to pay higher premiums and could be unable to afford the cost. They are a small minority of people currently in the Obamacare marketplaces, but more than a third of all people buying their own insurance, according to recent estimates. Higher premiums are also bad for taxpayers, since federal dollars help subsidize premiums for middle-income customers.
Possible solutions: Bring down costs instead of raising prices. More and more insurers are choosing to limit the number of doctors and hospitals they will cover in their plans. A lot of the reason that health insurance is so expensive in the United States is that doctors and hospitals charge more here than their counterparts in other countries. So the narrow network strategy may be a smart way to start getting different groups to negotiate down on their prices.

There are downsides to this strategy, of course. One is that it may be hard for patients who have complex health needs to find the care that they need with every plan. The other is that it could create a lot more disruptions in care for people, if they have to switch plans — and all their doctors — every year in order to get a good price on insurance. In the long run, insurers may have to find other ways to lower costs, like keeping customers healthier.
Another, simpler way to bring down prices would be to get more healthy people into the market, so the average insurance customer costs less, or use other tools to absorb the cost of people with complicated and expensive medical conditions. (See below.)
The market is too small
The problem: There are currently about half as many people in the exchanges as the Congressional Budget Office expected.
Why it’s a problem: About 27 million Americans still don’t have insurance, a bad thing by itself in a country where health insurance is often crucial to ensuring access to health care and protection from financial ruin. But too few customers also matter for the functioning of the market. Smaller markets make it hard for insurers to absorb the costs of a few sick patients. In some places — especially big cities — there are still enough people to spread out risk. But in many parts of the country, too few healthy people are signing up to balance the cost of those needing expensive medical care. And it means that, especially if a company is having trouble making money, there’s not a lot of upside to sticking around.
Possible solutions: Change the incentives, so more people who are currently uninsured buy health insurance. Hillary Clinton has talked about giving out more generous subsidies, so insurance costs less and more people can afford to buy it. Many Republican politicians suggest another way to lower prices: eliminating current requirements that insurance cover a wide array of services. Some policy experts, including Uwe Reinhardt, a Princeton health economist, in a recent Vox.com interview, have suggested tightening up the penalties for remaining uninsured, so people can’t wait and buy insurance only after they get sick.
A more controversial way to increase enrollment in the marketplaces would be to make employer coverage less attractive, so that more people who currently have insurance from work switch to buying their own. It was widely expected that this would happen as the law rolled out, but so far it hasn’t.
The rules are complicated
The problem: Some of the tools the federal government relied on to try to protect the insurance companies from large losses, especially in the early years, have not been as effective as the companies had hoped. The current rules ensure that a company doesn’t benefit from having healthier customers than its competitors, but doesn’t help insurers make up the losses when their overall premiums don’t cover their costs.
Why it’s a problem: If the insurers think the marketplace is unfair, or that there’s no way they can ever make money there, they are unlikely to participate. Because the health law relies on private companies to participate, conditions have to be favorable enough to keep them involved.
Possible solutions: The insurers that remain in the market — particularly many Blue Cross plans — have a long list of policy requests that would make their business less risky: by making it harder for sick people to buy coverage for short periods of time, by subsidizing the plans’ losses for very expensive patients, and in some cases by charging higher prices to older customers, who are more likely to be sick. But regulators have been cautious about embracing them, because such moves would shift financial risk to taxpayers and make it harder for people who need health care to get insurance.
The Obama administration has already made a few changes, including making it a little harder for people to sign up for insurance in the middle of the year. It has also signaled to Congress and state legislatures that a “reinsurance” program, which would pay insurers back for the sickest of their patients, would be a good idea.
There is little consensus among experts and advocates about what fixes would have the biggest impact when it comes to stabilizing the markets. The divides are not just partisan, but reflect persistent uncertainty about the most important things going wrong, and the most effective solutions to fix them.
Continue reading the main story


689 Comments
Readers shared their thoughts on this article.
The comments section is closed. To submit a letter to the editor for publication, write to letters@nytimes.com.
vandalfan
north idaho August 29, 2016Nonsense, the marketplace has worked perfectly, exactly the way the insurance companies wanted when they wrote the laws- they reap millions in taxpayers dollars.
Mark Marshall
Long Beach, CA August 29, 2016Insurance didn't come into existence for things that are definitely going to happen to people; it came into existence for things that might happen to people.
You might die early and unexpectedly, you might not; for that there is life insurance.
Your house may catch fire, ir may not; that's why you have fire insurance. And why fire insurance makes sense.
You may have an auto accident, you may not. Hence, insurance makes sense.
But there isn't anyone alive who will never have a health problem or never need to see a doctor. Insurance is therefore an illegitimate and inapropriate way of paying for this.
Single payor systems needn't have anything to do with altruism or citizens "looking out for each other". The other 99% of developed countries that have it aren't any more humanitarian than we are. Single payor's main virtue, and the only one that counts, is that it's sustainable and it works. For-profit insurance HAS no virtues. It neither works nor is sustainable, and is detested by the populace, as the endless post ACA damage reports have made all too clear.
JMC
Lost and confused August 29, 2016You left out the biggest problem, Bronze Policies are basically worthless due to their high deductibles, co-payments and limited coverage.
Bronze policies, are an illusion of coverage that make no sense for the vast majority of people in the lower third of the income strata.
Bubba Lew
Chicago August 29, 2016I hear people say all the time that young people are not buying health insurance because they are healthy. I have a friend who was young, healthy and quite robust, energetic and athletic. One day, he got a horrible pain in his stomach. 2 weeks later, he was diagnosed with Stage 4 pancreatic cancer. He had insurance, but I cringe when people say "healthy people do not need insurance" You are only healthy one day at a time. You never know when you will get hit by a car, get cancer, have a heart attack even if you feel well and healthy today. That is why we desperately need Universal Health Care in the US. Everyone will need a doctor sooner or later and we never know when.
Keith
USA August 29, 2016This idea of decreasing the salaries of physicians and hospital administrators is disconcerting. These individuals make up the second largest segment of the one percent. If we impoverish them then only CEOs and other managers will be rich, and they will rule our land. No one wants that. Freedom!!!
Helium
New England August 29, 2016The first goal of Obama Care was to provide subsidized insurance to the poor and sick with the cost picked up the the health/young/middle class. Second goal was to disincentivize the same health/young/middle class fro using health care themselves through higher co-pays and deductibles (poor/sick get receive subsidies for this as well but may still not be able to actuality use new insurance. Whoops!) Well there was some resistance once the cat was out of the bag and not enough paying and not using customers signed up. On to plan B. Perhaps Hillary will reveal it soon.
PaulB
Cincinnati, Ohio August 29, 2016Keep in mind that while health care economists and consumers are resurrecting talk of some kind of single payer system, the insurance lobby is hardly paying attention. And why should it? Assuming the Republicans maintain control of Congress (a reasonable supposition), there is no way in heaven or hell any legislation that even suggests a single payer option will ever see the light of day.
I'd wager that every person commenting on this article, the writers of the article, and the experts cited in the article already know that no such plan will ever come about unless the Democratic Party wins the White House and both houses of Congress this year or in some future year. It is not a health care issue, or a health insurance issue, or even a cost issue. It is an issue of political will.
Patriot
USA August 29, 2016The solution is lowering costs on health care providers. You do that with tort reform and reduced regulation not more lawyers and more regulation.
Jarvis
Greenwich, CT August 29, 2016"Then again, Europe doesn't pay obscene sums for militaristic stuff." With the U.S. footing the bill, you don't have to.
yankeegreg591
New York, NY August 29, 2016Suggest requiring insurers who want to participate in corporate health care coverage that to continue they must participate in public option at same rates for all.
Charles
N.J. August 29, 2016Re; obamacare - The time and costs to get to where we are today is unfathomable.
Here's a plan: A Kaiser - style healtcare for the entire country paid for by a 10% VAT and a 5% employee contribution. Cap medical at 15% GDP. In about a decade the bumps will be worked out and the problem is solved.
Debra Sayers
New York State August 29, 2016I enrolled in the Affordable Care Act in 2014. I am still with the same insurer.
My premium has risen, over two years , but not to the point that I can not
handle the increase. I opted out of my husband's employer's health care choice, and it was a wise decision. The Affordable Health Care Act provided me with an affordable choice.
However, health care should not be a for profit business. I stand with Senator
Bernie Sanders and his vision of Medicare for All, a single payer health care
system. Let's hope we can move in that direction in the years to come.
RM
is a trusted commenter Vermont August 29, 2016It was a half baked plan based on a proposal developed by the Heritage Foundation as a stalking horse proposal to derail a publicly run health insurance system for the public at large. As it was only a stalking horse proposal, when it was proposed in Congress, it had almost universal opposition from Republicans.
Our "friend" Senator Joe Liebermann from the insurance state of Connecticut put the kibosh on a public option. Now that he is out of there, its time to propose a public, single payer system based on Medicare.
Any system like Obamacare that tries to herd private insurance companies to write policies for people (those with prior conditions) whom they prefer to not do business with is bound to be complex and cumbersome And involuntary participants, both individuals and insurance companies, will resent it.
We need to do two things. One, replace Obamacare with a single payer system. And two, repeal the mandate that requires hospitals to treat people who cannot pay. After a few fools die who chose to not insure themselves, signing up for participation in the program will become a matter of choice.
Andrew Myers
Cambridge, MA August 29, 2016Now that Obamacare is going down the tubes, just as the Republicans predicted, the Democrats are bringing up "single payer" / "the public option", just as the Republicans predicted they would when it failed. But single payer has been tried already in the US, in Vermont. Vermont gave up on it because it was way too expensive. Vermont is a best case. If single payer can't work there, it can't work anywhere. Maybe it's time to start listening to the Republicans. They seem to have a better grasp on economics. Or at least they understand there is no such thing as a free lunch.
Doc J
Huntington Beach, CA August 29, 2016All the fixes here suggest fixing the ACA by more regulations and more tweaks by the Federal Government.
The assumption that the Government can manage such a monstrous process as national health insurance is the plain error.
Insurance is the business of "risk management". Do it well and you can make a profit. No all can insured. Do it not so well and your company is gone.
Health Insurance is different than Medical Care. Ask the Medical Community what are their solutions. Has anyone done that? Chalk Children's hospital charges nothing to people in need. Catholic Hospitals take all in need. Has anyone asked these people what they do? Many doctors, that I know, take off a few weeks to a month every year and donate their services. Has anyone asked them to help?
Get the Government out of the Health Care Insurance business period.
KBronson
Louisiana August 29, 2016The solutions are simple, but not easy, in that current rent seekers would be threatened and controllers would lose control. In the end the losers would be the government and private corporatists who wish to run other people's lives.
First we must accept that the solutions are plural-not a single plan. We are Americans and should seek solutions that strengthen American values of freedom, independence, and personal responsibility. Medicare works for the elderly. Non-Mandatory individual health markets that are national rather than state--we are a mobile people. Personal health savings accounts that can be started at birth and funded from a variety of sources with back up catastrophic insurance for most and enrollment in Medicare for the uninsurable chronically ill. Emergency care, a public utility, should be paid out of taxes and price regulated as no market mechanism can regulate prices where there is no choice.
James
Seattle, WA August 29, 2016This article is off track in so many ways. The discussion is always framed as a health insurance issue rather than a health care issue. The remainder of the industrialized world has figured that health care is a right but not here in America, where whether you live or die is a function of your privilege. And it's not merely the greed of our insurers; it's the greed of hospital CEOs, our pharmaceutical companies, our surgeons, the hedge funds that run our ambulance services, the advertisers who are paid millions to burnish the brands of our hospitals, and of course the ambulance chasing lawyers. Our system of medical care is effective if you can pay for it, but for tens of millions of people, it just stinks.
interesting how the writers comment that the public option is complicated and unworkable. Ever hear of Medicare? The only reason Medicare is complicated is because the health insurance companies are the middleman.
One solution to bringing down the costs to all would be to expand Medicare to include any persons with a chronic disease diagnosis such as cancer or any of the major chronic diseases such as diabetes, hypertension and cardiac disease. Removing that population from the private insurance pool would be a boon for both private insurers and the exchange itself. Many will say we can't pay for this but we do already. We pay for it in the form of free emergency care. Seeing a primary physician for preventative care is a far more cost effective option.
A Reader
US August 29, 2016After years of Times columnists insisting the ACA is working "just fine" and that "millions more Americans have coverage" ( though not actual access to affordable health care, but never mind), we finally see the denial beginning to recede in the face of overwhelming evidence that it is NOT working just fine. And the denial is only now receding because, with the ACA's inherent flaws on such vivid display right before the election, it's become politically necessary to acknowledge the reality. The fact that the insurance-company driven, hodge-podge, ill-fated ACA may have been the best that Obama and the Dems could manage to cram through Congress without a single Republican vote does not, unfortunately, make it a defensible program.
Ellen Liversidge
San Diego CA August 29, 2016Bernie was right.
Incremental tinkering just won't do it.
We need national healthcare, such as exists in every other Westernized nation. Bye bye, health insurance industry.
It's time to bite the bullet, or replace all of Congress and the Administration with politicians who will not take the payola.
frank G
california August 29, 2016It is just contraindicative to have a for profit industry in preserving life. I's Ghoulish.
Americans first right is the right to life.
Governments first responsibility is to protect the life of its citizens.
Profit motive has not provided better care or better delivery. It has just made several greedy industries rich until they have no restraint.
It's past time to treat health care in the special way we treat utilities. They get a profit based upon performance and delivery of services. They must provide services to all people within a unique territory. All liability is capped rather than litigated.
Most of the rest of the world figured this out long ago, and they enjoy superior health care overall. Our system survives on preying on the vulnerable in support of a few elites.
MiguelM
Fort Lauderdale, Fl. August 29, 2016Ha, like the unborn, oh right to choose.
RH
GA August 29, 2016The current mechanisms of health insurance coverage don't give the free market a chance. As long as every health care transaction is passed through middlemen, costs will be obscured and fabricated. Consumers need to see published prices for their doctors' services, just like they do at every other establishment where they spend money. True price competition is the only effective way to contain costs in the long term, and Obamacare does nothing to address that.
Eric Glen
Hopkinton NH August 29, 2016The law, as written, requires the redistribution of health insurance benefits among American voters. To work as designed the law requires those who played by the rules and had fared well under the prior system to relinquish their advantage. To, in effect, kick-in to the disadvantaged thereby enabling them to join the ranks of the insured. The laws proponents could not look their voters in the eye and admit this fundamental equation. Out of political expediency the law's proponents delayed or never enforced key provisions. The extra legal exemptions and delays postponed the day of reckoning but the day is nevertheless fast approaching. The Universal Health Care alternative would expand rather than diminish the volume of redistribution. Hillary will not allow her donor class to suffer such a fate. The fundamental truth remains, there is no such thing as a free lunch.
Don B
Massachusetts August 29, 2016Health insurance itself encourages constantly increasing prices for services. Making it mandatory just makes that worse. The moment Romney Care passed in Massachusetts, premiums started going up at double digit rates. Obama Care is the same thing, only worse.
We need a cost competitive market for healthcare products and services. The best bet is to get the young people off health insurance and let them shop for the services and products they need. Getting rid of the ban on drug importation will also help. Eventually we can get rid of employment based insurance and HMO style health insurance generally.
It doesn't make sense to start with the old and the sick. They can't afford our out of control prices or the premiums on a policy to pay for them. The only hope for them is outsourcing: flying to Belgium for their hip replacement, for example. American medicine is a luxury for the rich.
casual observer
Los angeles August 29, 2016Revise the legislation so that if a person is not enrolled in a full coverage plan (basic health care, including primary and urgent care, and hospitalization) then the person will automatically be enrolled in a pool of patients who will be assigned to insurers like automobile coverage for assigned risk, instead of fines or penalties. The rates can be determined with the companies by the public or private agency which does the assignments. That way all are covered without a public option which seems so horrible to Republicans and without any mandates, and insurers will have enough people enrolled to make it worthwhile.
Andrew Palfreyman
California August 29, 2016Why are Yanks so intent in shooting themselves continually in the foot? We solved this problem in Europe over 50 years ago. Just ask Bernie Sanders.
Then again, Europe doesn't pay obscene sums for militaristic stuff.
Melvin
SF August 29, 2016True enough.
You just let us pay for your defense, and then pontificate to us about our militarism.
August Velez
Florida August 29, 2016Then again, we also have to pay for your military defense, and our "healthcare spending" also includes the patent and copyrights -which helps pretend the European healthcare system is financially and morally responsible.
689 Comments
Readers shared their thoughts on this article.
The comments section is closed. To submit a letter to the editor for publication, write to letters@nytimes.com.